Our skin protects us from external influences every day. Walking barefoot or heavy use of the hands is enough to stimulate the formation of calluses. This is a completely natural process that makes the skin more resistant.
However, if excessive thickening occurs, very dry and hard areas of skin develop. These cases are referred to as hyperkeratosis.
When does hyperkeratosis occur?
The formation of corneas is a completely natural process to protect against external influences. It becomes problematic when too many callus cells are formed and do not detach quickly enough. The top layer of skin then thickens, the skin appears rough and can crack. This causes the skin to produce more keratin. This is a natural protein which, when overproduced, binds the cells together more strongly, resulting in thickened, dry, flaky skin.
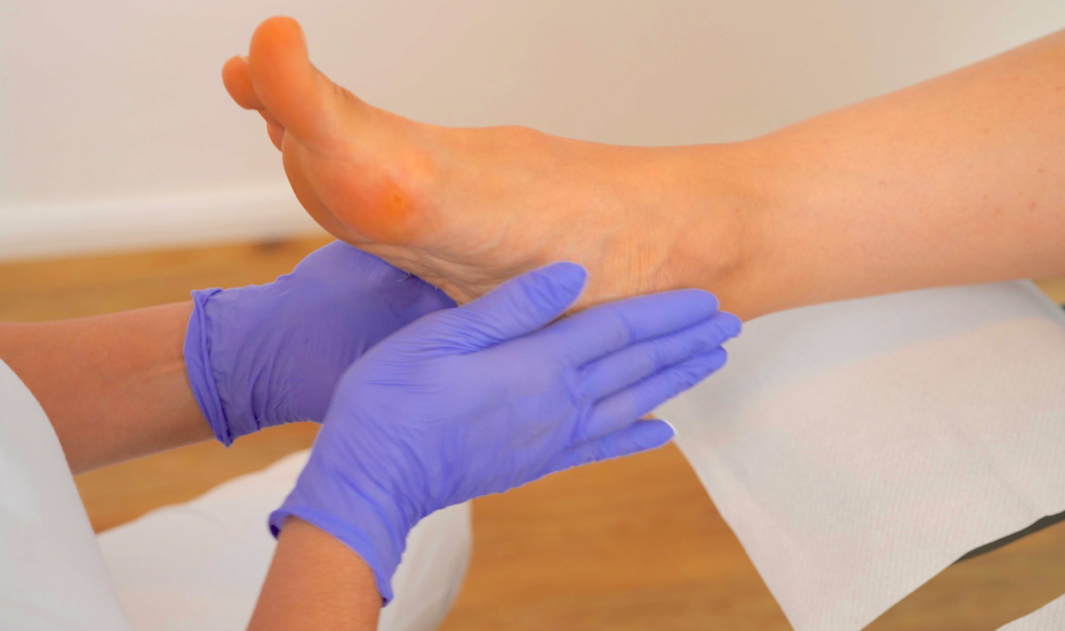
Hyperkeratosis can occur on areas of skin that are subject to high levels of stress. These include the palms of the hands, arms, legs and especially the soles of the feet. Podiatrists are familiar with this problem, as hyperkeratosis occurs quite frequently, especially on the feet.
If the keratinization takes on unhealthy characteristics , the doctor speaks of disorders and keratosis. Many people may also know it as chafing skin. In this case, a cosmetic problem becomes a case for the medical pedicure expert.
Symptoms and effects of hyperkeratosis
Hyperkeratosis can look very different depending on the cause and body part. Some forms are primarily a cosmetic issue, others can be painful and even promote inflammation.
Smooth hyperkeratosis
This form often occurs due to prolonged pressure or friction, for example from tight shoes or one-sided strain. The top layer of skin no longer regularly sheds old callus cells, so that thick, flat calluses gradually form. Affected areas feel rough, appear dry and lose elasticity.
Tearing hyperkeratosis
If thickened areas of skin become very dry, they can crack. This results in painful cracks, known as fissures or rhagades. These are not only unpleasant in everyday life, but also increase the risk of germs penetrating and causing inflammation. Therefore, such areas should be cared for particularly carefully to keep the skin elastic and resistant.
Keratosis pilaris (“chafing skin”)
In this form, the hair follicles become keratinized, resulting in small, rough nodules on the skin. They are easy to feel and are particularly noticeable on the upper arms and thighs. This makes the skin look uneven and is perceived as annoying by many sufferers. However, keratosis pilaris is usually medically harmless.
Calluses and corns
Calluses and corns are caused by repeated pressure or punctual friction, for example due to ill-fitting shoes or certain activities. Initially they develop unnoticed, but over time they can cause pain, particularly when walking or gripping. As they occur locally and are often sharply defined, they have a noticeable impact on everyday life and should not be ignored.
Possible causes
Hyperkeratosis usually develops as a result of a combination of different factors. Common triggers are
- Mechanical stress: Constant pressure or friction, for example from tight shoes, often leads to thickened skin on the feet and hands.
- Dry skin: If the skin lacks moisture, it becomes brittle. To compensate, it produces more horny cells.
- Occupational influences: Regular contact with tools, cleaning agents or chemicals stresses the skin and promotes calluses.
- Genetic factors and age: Some people have a greater tendency to keratinization due to hereditary factors. In addition, skin regeneration slows down with increasing age.
- Skin diseases and metabolic disorders: Psoriasis, eczema or diabetes can increase callus formation.
- Medication: Certain medications influence the skin’s metabolism and thus promote excessive keratinization.
Hyperkeratosis in diabetes
The metabolic disorder diabetes mellitus can impair the skin barrier and reduce the perception of pressure points. Calluses that have already formed are then often noticed too late and put under further pressure, which can lead to fissures, inflammation and subsequent complaints.
In many cases, the skin on the feet is affected. Pathogens often penetrate unnoticed, cause inflammation on fissures or pressure points and can lead to problems including diabetic foot syndrome. Comprehensive education and prevention can help here.
It is therefore particularly important that diabetics pay attention to proper foot care and take action in good time.
Act in good time and correctly
Urea (urea) is a natural moisturizing factor for the skin: it helps to bind water and prevent dryness. In higher concentrations, urea also supports the gentle removal of keratinized layers, making the skin feel smoother again.
The Spirularin SR chapped skin cream from Ocean Pharma also focuses on this. It provides intensive moisture and supports the skin barrier. The proven microalgae active ingredient Spiralin® also protects against external influences and promotes the regeneration of stressed areas.
Application tip: Initially use the chapped skin cream consistently for about two weeks. It is then advisable to switch to Spirularin® HF Mousse or Spirularin® HF Gel as maintenance care. This keeps the moisture better bound in the skin and prevents new, severe callus formation.
Do you have any questions? Feel free to send us an e-mail to: info@ocean-pharma.de. And if you would like to read more interesting tips, you can find them in our expert tips.
FAQ
Hyperkeratose bezeichnet eine übermäßige Verhornung der Haut. Sie entsteht, wenn mehr Hornzellen gebildet werden als sich ablösen, wodurch sich verdickte und trockene Hautstellen entwickeln.
Typische Anzeichen sind verdickte Haut, ein raues Hautgefühl, gelbliche oder weißliche Verfärbungen sowie schmerzhafte Risse (Schrunden).
Zu den häufigsten Ursachen zählen mechanische Belastung (z. B. durch enge Schuhe), trockene Haut, genetische Veranlagung, Hauterkrankungen wie Schuppenflechte oder berufliche Beanspruchung.
Regelmäßige Pflege mit feuchtigkeitsspendenden Produkten, sanftes Entfernen überschüssiger Hornhaut sowie bequemes Schuhwerk können helfen, die Haut gesund zu halten.
Am häufigsten sind Füße, Fersen und Ballen betroffen, da diese Bereiche stark belastet werden. Aber auch Hände, Ellenbogen oder andere beanspruchte Stellen können betroffen sein.
Image source: ocean pharma GmbH
Experten-Tipp entstand in Zusammenarbeit mit:

Anke Niederau
Anke Niederau has been self-employed in medical foot care since 1990. Among other things, she has completed further training on the subject of "reflexology work on the foot" and as a diabetic podiatrist DDG. She is also the author of the bestseller "Das große Buch der Nagelerkrankungen".
Until 2005, she worked as a lecturer in medical foot care at the Düsseldorf Chamber of Crafts and until 2006 as a teacher at the Kaiserswerther Diakonie specialist school for podiatry. Since 2007, the author has worked as a freelance lecturer at various podiatry and chiropody schools.